Osteoarthritis (OA)

MBChB (New Zealand), PGDipObstMedGyn, FRACP (New Zealand), FAMS (Rheumatology)
Osteoarthritis develops when the protective cartilage that cushions the ends of bones gradually breaks down. Ageing is the most important risk factor. Over time, cartilage becomes thinner, less elastic and less able to absorb shock within the joint. As the cartilage wears away, the bones may begin to rub against each other during movement, leading to pain, stiffness and reduced mobility. Other contributing factors include:
Previous joint injuries, such as ligament tears or meniscus damage, can increase the risk of developing osteoarthritis later in life.
Excess body weight places added stress on weight-bearing joints, particularly the knees and hips, which can accelerate cartilage wear and joint degeneration.
Some individuals may inherit genes that make them more likely to develop osteoarthritis.
Certain occupations or sports that place repetitive stress on a joint can increase the risk of developing osteoarthritis over time. Activities that involve frequent twisting, heavy lifting or high- impact movements can gradually wear down cartilage.
Abnormal joint mechanics can place uneven stress on the joints, making them more prone to accelerated cartilage breakdown and increasing the risk of osteoarthritis.
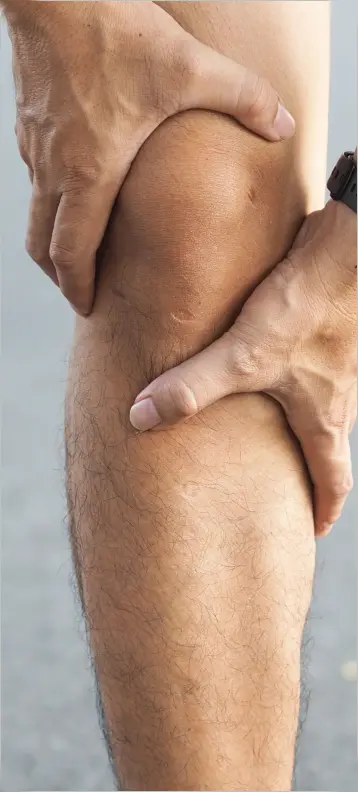
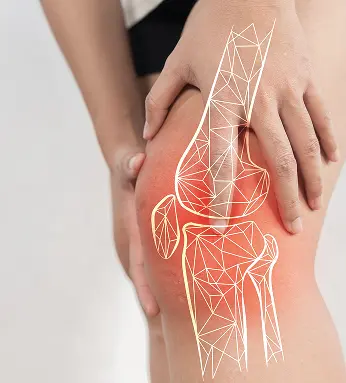
The symptoms of osteoarthritis typically develop gradually and may vary in severity over time. Early symptoms often include joint pain and stiffness, especially after activity or at the end of the day.
Joint Pain and Stiffness Pain commonly affects the knees, hips, hands or spine. Stiffness is often more noticeable after periods of rest or upon waking. Symptoms may flare or worsen following prolonged activity or overuse of the joint.
Reduced Flexibility As cartilage wears away, joints may become less flexible, making it difficult to bend, straighten or fully use the affected joint during everyday activities.
Swelling and Tenderness Mild swelling can occur due to inflammation or fluid build-up within the joint. The area may feel tender when gentle pressure is applied.
Grinding Sensation Some people may experience a grating or clicking sensation during movement, caused by changes in the joint surfaces.
Joint Instability In weight-bearing joints such as the knees, one may experience a feeling of instability or that the joint is giving way.
Osteoarthritis is usually diagnosed through a combination of clinical assessment and imaging tests. Because joint pain can have many causes, a structured evaluation is essential to confirm the diagnosis and guide appropriate management.
Diagnosis begins with a detailed discussion of your symptoms, including when the pain occurs, the duration of stiffness and how it impacts your daily activities. During the physical examination, the doctor will check for joint tenderness, swelling and range of motion, as well as signs such as crepitus or joint instability.
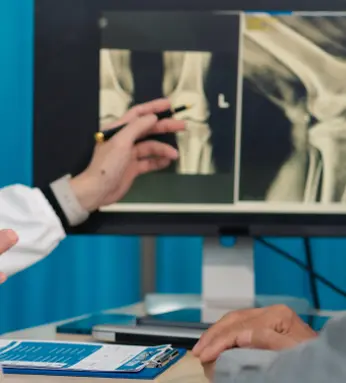
X-rays are commonly used to identify changes associated with osteoarthritis, such as joint space narrowing, bone spurs or changes in bone structure. In some cases, an MRI may be recommended to provide detailed images of cartilage and surrounding soft tissues, particularly when X-rays do not fully explain the symptoms.
How Do Rheumatologists Treat Osteoarthritis?
Treatment of osteoarthritis focuses on relieving pain, improving joint function and supporting long-term mobility. Management is tailored based on the severity of symptoms, the joints affected and your individual lifestyle needs.
Lifestyle measures form the foundation of osteoarthritis care and are a key part of long-term management. This includes:

Activities such as walking, swimming, strength training or cycling help strengthen the muscles around the joint, improve flexibility and reduce pain.

Maintaining a healthy weight is particularly important for knee and hip osteoarthritis, as excess body weight increases stress on these joints. Even modest weight loss can improve symptoms and joint function.

Modifying repetitive or high-stress movements and balancing activity with regular periods of rest can help reduce flare-ups.
Medical management aims to relieve pain, reduce inflammation and support day-to-day function, while taking into account your overall health profile and treatment preferences.

NSAIDs are commonly used to relieve joint pain and reduce inflammation in osteoarthritis. They can help improve comfort and mobility.

Corticosteroid injections in the affected joint may be considered for persistent pain or flare-ups. They help reduce inflammation and provide short-term symptom relief.
Physiotherapy is essential for maintaining joint strength, stability and range of motion. A structured programme tailored to your condition can support long-term function and mobility.
Our Rheumatologist
Dr Poh Yih Jia
Senior Consultant Rheumatologist
Dr Poh Yih Jia is a senior consultant rheumatologist with more than 20 years of medical experience in
New Zealand and Singapore. She has extensive experience in the diagnosis and management of degenerative
and inflammatory joint conditions, including osteoarthritis.
Her commitment to patient-centred care has earned her multiple accolades, including the Singapore Health
Quality Service Award and the Service with a Heart Award. She remains dedicated to advancing
rheumatology through clinical practice, education and research, ensuring her patients receive the most
current, evidence-based care for osteoarthritis and other rheumatic conditions.

FAQs on Osteoarthritis (OA)
Osteoarthritis is a degenerative joint condition in which the protective cartilage between bones gradually wears down. While ageing is the main risk factor, previous joint injuries, excess body weight, repetitive joint stress and genetic predisposition can also increase the likelihood of developing the condition.
Osteoarthritis often causes joint pain that worsens with activity, stiffness after periods of rest and reduced flexibility. Symptoms usually develop gradually and commonly affect the knees, hips, hands or spine. A clinical evaluation, sometimes supported by X-rays, is used to confirm the diagnosis.
Osteoarthritis cannot be cured, as cartilage cannot fully regenerate. However, its symptoms can be effectively managed. With the right combination of lifestyle measures, physiotherapy and medical treatment, many people are able to maintain mobility and continue daily activities independently.
If left unmanaged, osteoarthritis may lead to increased pain, reduced mobility and difficulty with daily activities. In advanced stages, joint deformity or significant functional limitations may develop. Early management can help relieve symptoms and reduce the risk of long-term disability.
While osteoarthritis cannot always be prevented, certain measures may reduce risk or slow progression. Maintaining a healthy weight, staying active with regular low-impact exercise and avoiding repetitive joint strain can support joint health. Early assessment and appropriate management of joint injuries may also help preserve long-term function.


