Psoriatic
Arthritis (PsA)

MBChB (New Zealand), PGDipObstMedGyn, FRACP (New Zealand), FAMS (Rheumatology)
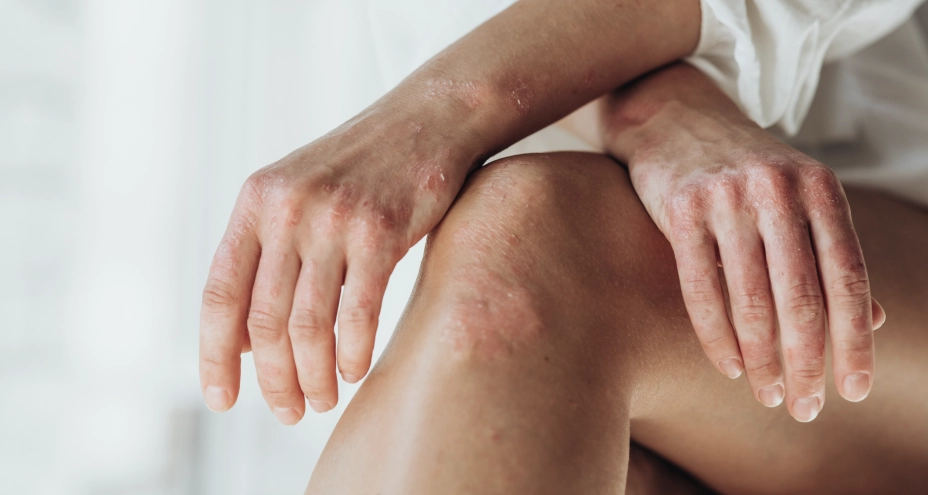
Psoriatic arthritis is a chronic inflammatory condition that affects the joints and may occur in people with psoriasis, an autoimmune skin condition that causes scaly, red patches. It can cause joint pain, stiffness and swelling. While it often affects the larger joints such as the knees and shoulders, it can also involve the fingers, toes, tendons or spine.
Without appropriate treatment, persistent inflammation can lead to progressive joint damage and reduced function. Early diagnosis and timely treatment can help control psoriatic arthritis, preserve joint function and support an active, fulfilling life. At the Centre for Rheumatology & Arthritis, Dr Poh works closely with you to understand your symptoms and tailor a treatment plan that supports long-term joint health and overall well-being.
Psoriatic arthritis is an autoimmune condition in which the immune system mistakenly attacks the joints and surrounding tissues, causing inflammation. Its exact cause is not fully understood, but it is thought to result from a combination of genetic and environmental factors.
Most people who develop psoriatic arthritis have a history of psoriasis, although in some cases, joint symptoms may appear before skin changes.
A genetic predisposition increases the likelihood of developing the condition.
Psoriatic arthritis commonly develops between the ages of 30 and 50, although it can occur at any age.
In people who are susceptible, infections or physical trauma may trigger the onset of psoriatic arthritis.
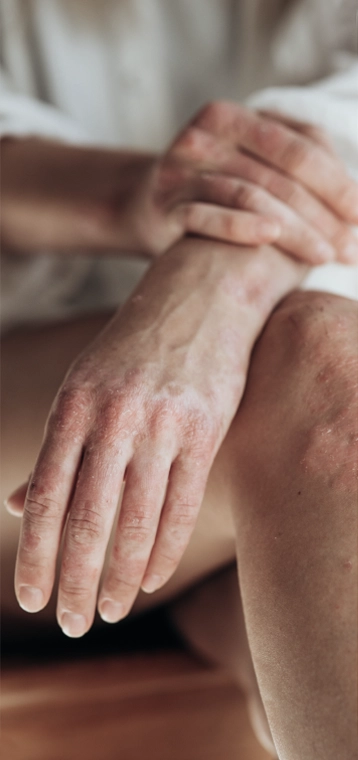
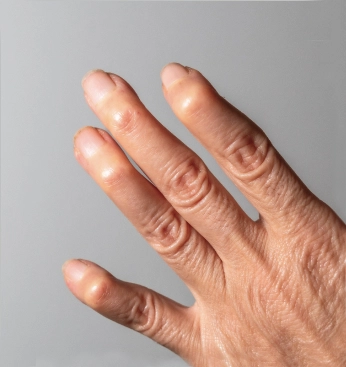
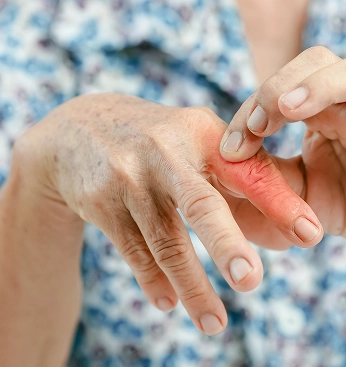
The symptoms of psoriatic arthritis can vary widely and may come and go over time. Some people experience mild joint discomfort, while others have persistent inflammation affecting multiple joints.
Joint Pain and Swelling Pain, stiffness and swelling may affect the fingers, toes, knees, ankles or other joints. Symptoms are often more pronounced in the morning or after periods of inactivity.
Dactylitis (“Sausage” Digits) Whole fingers or toes may become swollen, giving a “sausage-like” appearance due to inflammation of the joints and surrounding tendons.
Enthesitis Inflammation where tendons and ligaments attach to bone can cause pain, commonly at the heels or soles of feet.
Spinal Involvement Some individuals develop stiffness and pain in the lower back.
Nail Changes Fingernails and toenails may develop small indentations called pits. The nails may become brittle or start to lift away from the nail bed.
Diagnosing psoriatic arthritis can be challenging, particularly in the early stages, as symptoms may resemble other forms of inflammatory arthritis. A comprehensive evaluation is essential to confirm the diagnosis and guide appropriate treatment.
Assessment begins with a detailed discussion of your joint symptoms. During the examination, the doctor will assess for joint swelling and tenderness, tendon inflammation and nail changes which can help support the diagnosis.
X-rays, ultrasound or MRI scans may be recommended to detect joint inflammation or structural changes.
Blood tests may be performed to assess levels of inflammation and to exclude other conditions.
How Do Rheumatologists Treat Psoriatic Arthritis?
Treatment for psoriatic arthritis aims to reduce inflammation, prevent joint damage and preserve long-term function. Management is personalised based on the pattern and severity of joint involvement, the presence of skin disease and your overall health needs.

NSAIDs can help relieve joint pain, swelling and stiffness, particularly during flare-ups.

These medications help to prevent joint damage and slow disease progression.

Biologic and targeted synthetic DMARDs work by targeting specific pathways in the immune system that drive inflammation, offering more precise control of psoriatic arthritis. These treatments can also help reduce the risk of long-term joint damage.
Physiotherapy plays an important role in the management of psoriatic arthritis by helping to maintain joint mobility, improve muscle strength and support overall physical function. A tailored programme can teach practical techniques and targeted exercises to reduce strain on affected joints, making everyday activities easier and more comfortable.
Although psoriatic arthritis is a long-term condition, adopting practical lifestyle measures can play a key role in managing symptoms, protecting joint health and supporting overall well-being.
Regular physical activity helps maintain joint flexibility, muscle strength and overall mobility. Low-impact activities such as walking, swimming or cycling can be particularly beneficial. Incorporating gentle stretching and targeted strengthening exercises may help support joints affected by inflammation and improve function.
Maintaining a healthy weight can help reduce stress on weight-bearing joints and may enhance response to treatment. Following a balanced, nutritious diet supports overall health, energy levels and long- term well-being.
Being mindful of repetitive strain and high-impact activities can reduce unnecessary stress on inflamed joints. Making simple adjustments to daily routines may also help minimise discomfort, particularly during flare-ups.
Ongoing care for psoriasis, including adherence to prescribed treatments, is an important part of comprehensive disease management.
Our Rheumatologist
Dr Poh Yih Jia
Senior Consultant Rheumatologist
Dr Poh Yih Jia is a senior consultant rheumatologist with over 20 years of medical experience in New Zealand and Singapore. She has extensive experience in the diagnosis and management of autoimmune diseases and inflammatory joint conditions, including psoriatic arthritis.
Her commitment to patient-centred care has earned her multiple accolades, including the Singapore Health Quality Service Award and the Service with a Heart Award. She remains committed to delivering current, evidence-based care to patients with psoriatic arthritis and other rheumatic diseases.

FAQs on Psoriatic Arthritis
Psoriatic arthritis is a chronic autoimmune condition in which the immune system causes inflammation in the joints and surrounding tissues. It commonly occurs in individuals with psoriasis. Both genetic predisposition and environmental factors, such as infections, may contribute to its development.
Common symptoms include joint pain, swelling and stiffness, particularly in the fingers, toes or lower back. Some people may also develop dactylitis (“sausage-like” swelling of the fingers and toes), heel pain or nail changes. If you have psoriasis and experience joint symptoms, it is advisable to seek medical evaluation.
While psoriatic arthritis cannot be cured, it can be effectively managed with appropriate care. Early diagnosis and timely treatment help control inflammation, relieve symptoms and prevent joint damage. With the right care, many individuals are able to lead active and fulfilling lives.
Without treatment, persistent inflammation can lead to progressive joint damage, deformity and reduced mobility. Early and effective treatment is key to minimising the risk of long-term functional impairment.
There is currently no proven way to prevent psoriatic arthritis. However, early recognition of joint symptoms in individuals with psoriasis enables prompt treatment. Effective control of inflammation will help reduce the risk of joint damage and long-term complications.